A Complete Guide to Understanding the Cataract Removal Procedure
Cataracts are one of the most common age-related eye conditions, affecting millions of people worldwide. This clouding of the eye's natural lens can gradually impair vision, making everyday activities like reading, driving, or recognizing faces increasingly difficult. Fortunately, cataract removal is a well-established, highly successful procedure that restores clear vision for countless individuals each year. Understanding what cataracts are, how they are removed, and what to expect during recovery can help ease concerns and prepare you for the journey toward improved sight.
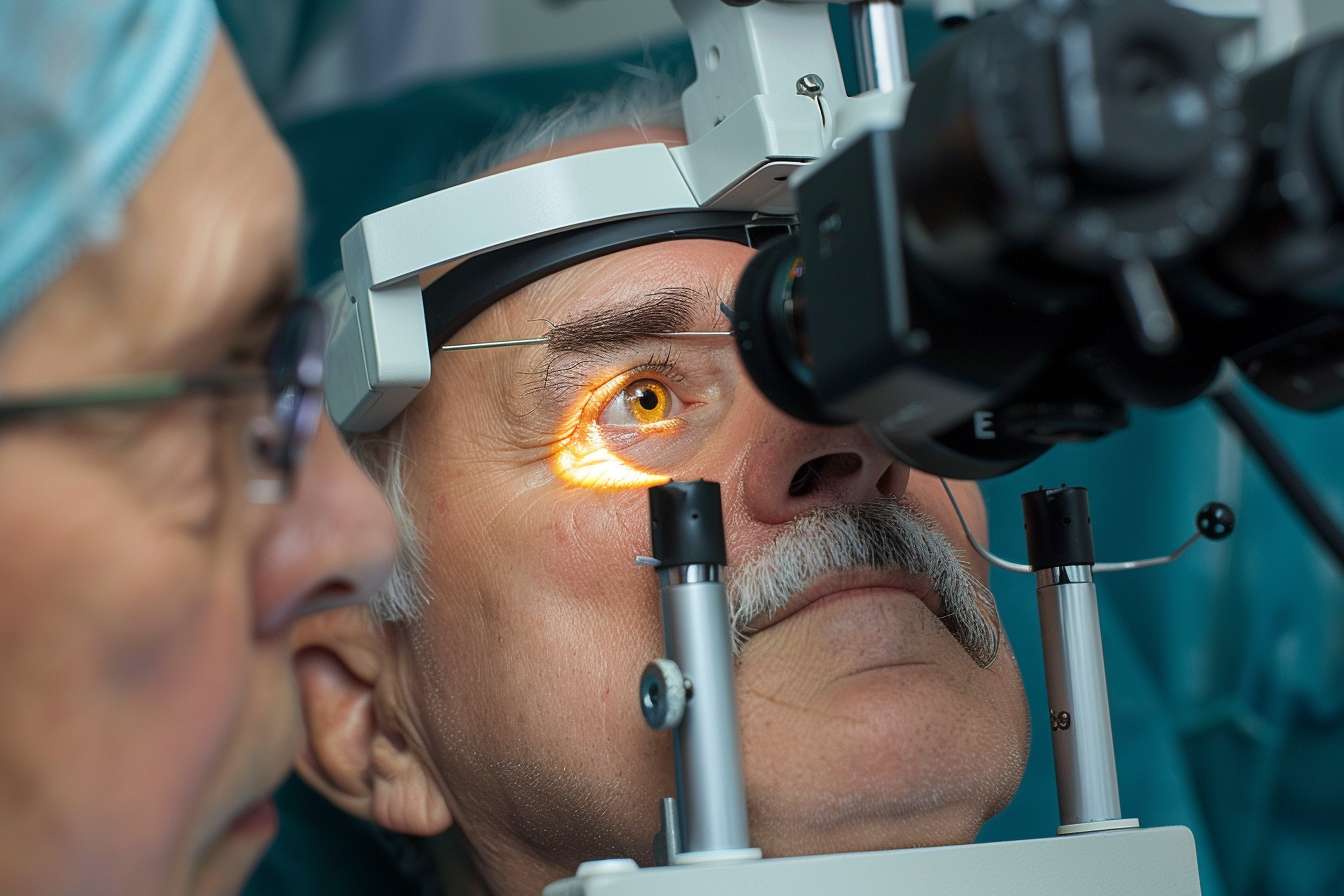
Cataracts develop when proteins in the eye’s lens break down and clump together, creating cloudy areas that block or distort light entering the eye. This natural lens sits behind the iris and pupil, focusing light onto the retina at the back of the eye. As cataracts progress, vision becomes increasingly blurred, colors may appear faded, and glare from lights can become bothersome. While cataracts typically develop slowly over years, they eventually reach a point where surgical intervention becomes necessary to restore functional vision.
What Exactly is a Cataract?
A cataract is not a growth or film over the eye, but rather a clouding within the lens itself. The lens is primarily composed of water and proteins arranged in a precise way to keep the lens clear. With age, these proteins can deteriorate and cluster together, forming opaque regions. Risk factors include aging, prolonged ultraviolet light exposure, diabetes, smoking, certain medications like corticosteroids, and previous eye injuries or surgeries. Most cataracts are age-related and develop gradually, though congenital cataracts can occur in infants, and traumatic cataracts may form after eye injuries. Symptoms include blurry or dim vision, difficulty seeing at night, sensitivity to light and glare, seeing halos around lights, frequent changes in eyeglass prescriptions, and fading or yellowing of colors.
The Step-by-Step Removal Process
Cataract surgery is one of the most commonly performed and safest surgical procedures worldwide. The operation typically takes 15 to 30 minutes and is usually performed on an outpatient basis under local anesthesia. The most common technique is phacoemulsification, where the surgeon makes a tiny incision in the cornea, inserts an ultrasound probe that breaks up the cloudy lens into small fragments, and then suctions out these pieces. Once the natural lens is removed, an artificial intraocular lens is implanted in its place to restore clear vision. This synthetic lens is designed to remain in the eye permanently and requires no maintenance.
Before surgery, the eye is numbed with anesthetic drops, and the patient remains awake but relaxed throughout the procedure. The surgeon uses a microscope to view the eye and performs the operation with precision instruments. After the cloudy lens is removed and the new lens inserted, the small incision typically seals itself without stitches. In some cases, a slightly larger incision may be needed, requiring one or two sutures. Patients usually experience minimal discomfort during the procedure and can return home the same day with protective eyewear and detailed aftercare instructions.
The Recovery Phase
Recovery from cataract surgery is generally quick and straightforward for most patients. Vision may be blurry immediately after the procedure as the eye adjusts to the new lens and heals from the surgery. Many people notice significant improvement within a few days, though complete healing can take several weeks. During the initial recovery period, patients are prescribed antibiotic and anti-inflammatory eye drops to prevent infection and reduce inflammation. It is crucial to follow the medication schedule precisely and attend all follow-up appointments with the ophthalmologist.
During recovery, certain precautions help ensure optimal healing. Patients should avoid rubbing or pressing on the eye, refrain from strenuous activities and heavy lifting for at least a week, wear protective eyewear as directed, keep water and soap out of the eye while showering, and avoid swimming or hot tubs for several weeks. Mild discomfort, itching, or light sensitivity is normal, but severe pain, sudden vision loss, or increasing redness should be reported to the doctor immediately. Most patients can resume normal activities, including reading and watching television, within a few days, though driving should wait until cleared by the surgeon.
Cost Considerations and Provider Options
The cost of cataract surgery varies significantly depending on location, the type of intraocular lens chosen, and whether the procedure is covered by insurance. In countries with public healthcare systems, cataract surgery may be fully covered, while private patients or those in countries without universal coverage may face out-of-pocket expenses. Standard monofocal lenses are typically covered by insurance, while premium lenses that correct astigmatism or provide multifocal vision usually require additional payment.
| Provider Type | Services Offered | Cost Estimation |
|---|---|---|
| Public Hospital | Standard cataract removal with monofocal lens | Often fully covered by insurance or $0-$1,500 per eye |
| Private Clinic | Standard or premium lens options, faster scheduling | $3,000-$5,000 per eye without insurance |
| Academic Medical Center | Advanced techniques, research-based care | $2,500-$4,500 per eye, insurance may apply |
| Specialized Eye Surgery Center | Laser-assisted surgery, premium lens selection | $4,000-$6,000 per eye, premium features extra |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Frequently Asked Questions
Many patients wonder whether cataract surgery is painful. The procedure itself is not painful due to effective anesthesia, though some pressure or mild discomfort may be felt. Afterward, the eye may feel scratchy or slightly sore for a day or two, but significant pain is uncommon. Another common question involves how long the artificial lens lasts. Intraocular lenses are designed to be permanent and typically last a lifetime without needing replacement or maintenance.
Patients also ask about the possibility of cataracts returning after surgery. Once the natural lens is removed, cataracts cannot redevelop in that lens. However, some people experience posterior capsule opacification, where the membrane holding the artificial lens becomes cloudy. This condition, sometimes called a secondary cataract, can be easily treated with a quick, painless laser procedure. Regarding both eyes, cataracts often develop in both, but surgery is typically performed on one eye at a time, with several weeks between procedures to allow the first eye to heal.
Cataract removal is a transformative procedure that has restored vision and improved quality of life for millions of people. With modern techniques, high success rates, and relatively quick recovery times, it remains one of the most effective treatments in ophthalmology. Understanding the nature of cataracts, the surgical process, and what to expect during recovery empowers patients to make informed decisions and approach the procedure with confidence. If you are experiencing symptoms of cataracts, consulting with a qualified eye care professional is the essential first step toward clearer vision.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.




