5 Common Medications Used to Treat Eczema Effectively
Eczema, also known as atopic dermatitis, affects millions of people in the United States, causing uncomfortable symptoms like itching, redness, and inflammation. Managing this chronic skin condition often requires a combination of treatments tailored to individual needs. Understanding the most commonly prescribed medications can help patients work more effectively with their healthcare providers to find relief and minimize flareups.
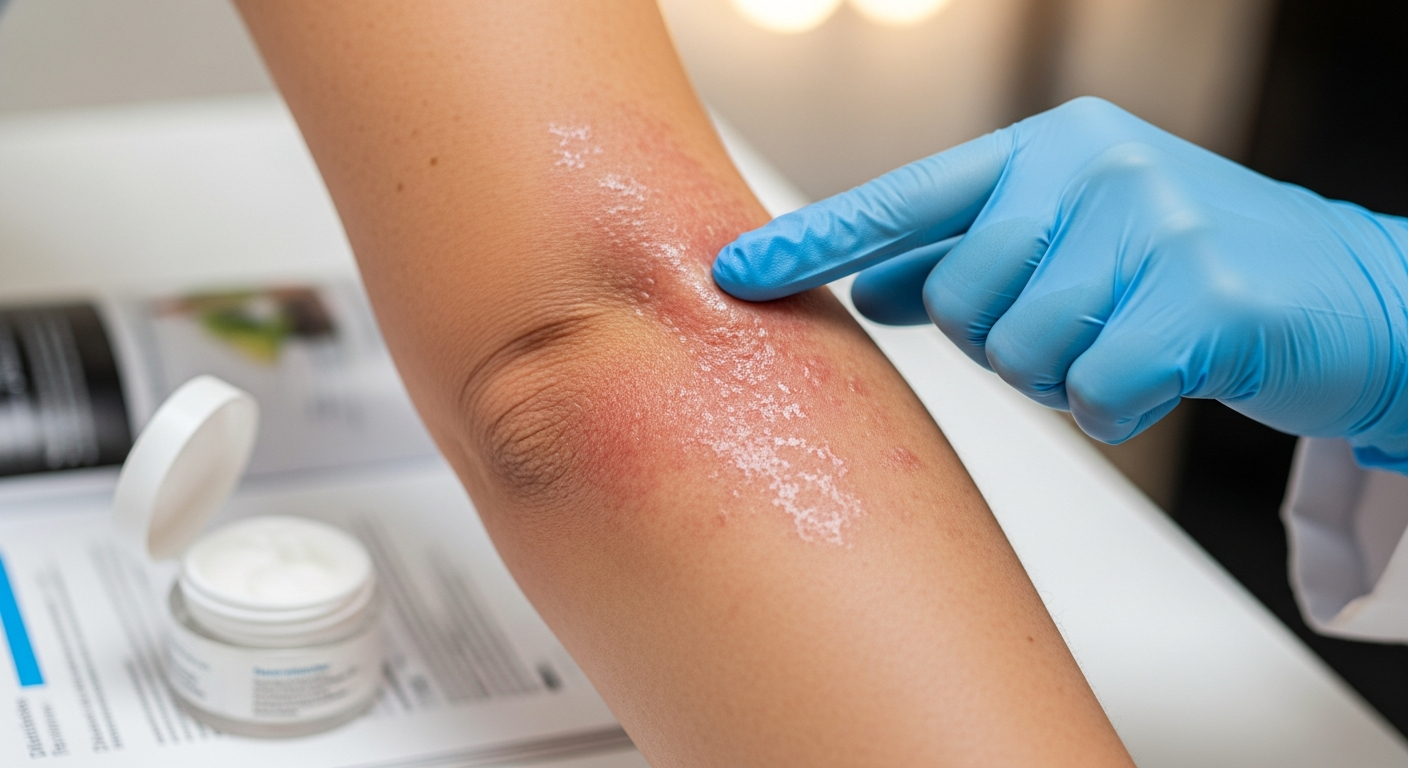
Living with eczema means dealing with persistent skin irritation that can significantly impact daily life. While there is no cure for this chronic condition, various medications have proven effective in managing symptoms and reducing the frequency of flareups. These treatments range from over-the-counter options to prescription-strength medications, each serving specific purposes in an overall management plan.
How Do Topical Corticosteroids Help Control Inflammation?
Topical corticosteroids remain the most widely prescribed medications for eczema treatment. These creams and ointments work by reducing inflammation and suppressing the immune response that causes skin irritation. Available in varying strengths from mild to very potent, corticosteroids are typically applied directly to affected areas during flareups. Mild formulations may be used on sensitive areas like the face, while stronger versions treat more severe symptoms on the body. Healthcare providers usually recommend using these medications for short periods to minimize potential side effects such as skin thinning. When used as directed, topical steroids provide significant relief for most patients with atopic dermatitis.
What Role Do Calcineurin Inhibitors Play in Therapy?
Calcineurin inhibitors represent a non-steroidal alternative for managing eczema symptoms. These prescription medications, available as creams or ointments, work by suppressing specific immune system activities that trigger inflammation. Unlike corticosteroids, calcineurin inhibitors can be used for longer periods without causing skin thinning, making them particularly suitable for sensitive areas. They are often prescribed when steroids are ineffective or inappropriate for certain body locations. Patients may experience a temporary burning sensation when first applying these medications, but this typically subsides with continued use. These topical treatments have become valuable options in long-term eczema management strategies.
Can Antihistamines Provide Relief from Itching?
Antihistamines are frequently recommended to help manage the intense itching associated with eczema. While they do not directly treat the underlying inflammation, these medications can reduce the urge to scratch, which often worsens skin damage and leads to infection. Both over-the-counter and prescription antihistamines are available, with some formulations causing drowsiness that may help patients sleep despite nighttime itching. Healthcare providers may suggest taking these medications in the evening to maximize rest and minimize daytime sedation. Antihistamines work best as part of a comprehensive treatment plan that includes topical medications and proper skin care routines.
When Are Immunosuppressants and Biologics Necessary?
For moderate to severe eczema that does not respond adequately to topical treatments, systemic medications may be required. Immunosuppressants work throughout the body to reduce immune system activity that triggers skin inflammation. These prescription medications require careful monitoring by healthcare providers due to potential side effects. Biologics represent a newer class of therapy that targets specific proteins involved in the inflammatory process. Administered through injection, biologics have shown remarkable effectiveness for patients with severe atopic dermatitis. These advanced treatments are typically reserved for cases where other medications have failed to provide sufficient relief.
| Medication Type | Common Examples | Primary Function | Typical Cost Range |
|---|---|---|---|
| Topical Corticosteroids | Hydrocortisone, Triamcinolone | Reduce inflammation and itching | $15-$200 per tube |
| Calcineurin Inhibitors | Tacrolimus, Pimecrolimus | Non-steroidal inflammation control | $300-$600 per tube |
| Antihistamines | Diphenhydramine, Cetirizine | Relieve itching and improve sleep | $5-$30 per bottle |
| Immunosuppressants | Cyclosporine, Methotrexate | Systemic immune suppression | $100-$500 monthly |
| Biologics | Dupilumab | Target specific inflammatory proteins | $3,000-$3,500 monthly |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Why Are Moisturizers and Emollients Essential for Management?
While not technically medications, moisturizers and emollients form the foundation of any effective eczema treatment plan. These products help restore and maintain the skin barrier, preventing moisture loss that worsens symptoms. Thick ointments generally provide better protection than lighter creams or lotions, especially for severely dry skin. Regular application, particularly immediately after bathing, helps lock in moisture and reduces the need for stronger prescription medications. Many dermatologists recommend using fragrance-free, hypoallergenic products to avoid additional irritation. Consistent use of quality moisturizers can significantly reduce flareup frequency and severity, making them an indispensable component of long-term eczema management.
Managing eczema effectively requires understanding the various medication options available and working closely with healthcare providers to develop a personalized treatment strategy. From topical corticosteroids and calcineurin inhibitors to antihistamines and advanced biologics, each medication type serves specific purposes in controlling symptoms and improving quality of life. Combined with proper skin care routines and trigger avoidance, these medications help millions of people successfully manage their atopic dermatitis and minimize the impact of this chronic condition on their daily activities.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.